Healthy Calf Conference
Follow to stay up-to-date on all Healthy Calf Conference updates. Speaker announcements, sponsorship information, registration announcements, and more.
By Cynthia Miltenburg, DVM, DVSc.
Lead Veterinarian Animal Health and Welfare
Ontario Ministry of Agriculture, Food & Rural Affairs
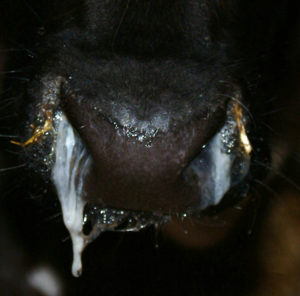
The cattle adapted strain of Salmonella known as Salmonella Dublin is becoming increasingly prevalent in Ontario. Surveillance data reported by the Animal Health Laboratory in Ontario indicates that positive diagnostic samples continue to be identified from new premises each month. What does this mean for my operation? For premises that remain infection free, the risk of acquiring the disease is increasing. This is particularly true for veal operations that receive calves from a variety of sources that may be changing over time.
Salmonella Dublin is a bacterial disease caused by Salmonella enterica subsp. enterica serovar Dublin. This bacterium can cause serious disease in cattle with high mortality and the potential to infect humans, too. The disease came to the forefront when highly resistant strains were first detected in Quebec in 2011 and Ontario in 2014. Calves become infected when they ingest the bacteria that is shed through manure, urine, milk, saliva, semen, or vaginal discharge. The most common signs of disease are fever, pneumonia that is unresponsive to treatment, and rapid, high mortality. Unlike other Salmonella strains, diarrhea is not a consistent sign. Clinical signs are typically seen in animals less than six months of age although older cattle can be affected. Once infected, those that survive can become persistent shedders or shed periodically, continually contaminating the environment. This intermittent shedding pattern makes testing animals and establishing them as disease negative difficult.
Testing of samples submitted to laboratories in Ontario, Quebec and New York have consistently identified strains of Salmonella Dublin that are multi-drug resistant. Isolates collected at the Animal Health Laboratory in Ontario between 2014 and 2018 have been found to be resistant to four to five different classes of antibiotics. As this resistance provides few to no treatment options when disease outbreaks occur, it therefore necessitates disease prevention.
Livestock producers also need to be aware that all Salmonella infections have the potential to infect people, other livestock and companion animals, causing illness. Salmonella Dublin can be very serious and has a higher mortality rate in people than other Salmonella serovars. Calf handlers, farm workers and their families are at risk of infection during an outbreak through exposure to infectious bodily excretions. People with a weakened immune system, pregnant women, the very young and elderly are especially susceptible to illness. For those handling sick calves, changing clothing and observing proper hand-washing practices are critical. Proper protective equipment such as a mask and goggles, gloves and over suit should be worn when cleaning infected areas. As Salmonella can be shed in milk, consumption of raw milk is a high-risk practice as well. If any animal caretakers show signs of serious illness, notify a physician.

The major goal for most operations which have had no infections to date is to keep Salmonella Dublin out. Once disease enters the premise it can be an ongoing struggle to maintain healthy cattle. Risk factors for the introduction of Salmonella Dublin are animal movement and animal transport; two factors that are significant in veal production. Prohibiting entry of disease involves practicing stringent biosecurity and sourcing animals from reliable sources. Any calves that come from an unknown farm or dealer should be considered high risk for introducing infection. This includes cattle entering from out-of-province or those that have visited a sales yard. Even well-known sources of calves can be carriers of Salmonella Dublin and introduce infection. Regular communication with source farms about disease and mortality, and preventative practices if possible is ideal. Calves that were not born into a clean maternity area or received inadequate colostrum will be more susceptible to disease.
Another risk for infection occurs when uninfected cattle are moved in a vehicle or trailer that has been insufficiently cleaned after transporting infected cattle. Proper cleaning requires removal of all bedding and feces, disinfecting the vehicle and re-bedding. This standard should be expected of all drovers or personnel that transport cattle on your behalf. Ensuring that all visitors wear clean clothing and boots will also reduce risk of introduction. Likewise, do not wear the same clothing and boots while visiting other facilities that you wear when caring for your own animals.
Any time a change in mortality is noted, prompt investigation can help determine the cause and limit the extent of the outbreak. When Salmonella Dublin is introduced to a previously naïve herd, mortality can quickly become very high. Where possible, isolating newly purchased calves from other calves already on the farm can prevent the introduction or spread of disease should it be introduced.
Immediately identifying and isolating sick animals and following strict hygiene protocols is necessary to reduce disease spread. Feeding equipment should not be shared between sick and healthy animals which makes group feeding particularly difficult to manage. If group feeding is necessary, small groups are recommended. Scrapers, shovels and other tools can spread the bacteria to a previously uncontaminated area and should not be shared. As the bacteria is shed in manure, it is important to wash or change boots between groups of cattle. Salmonella can be aerosolized so attention to air movement and ventilation in the barn is important. This is a risk if pressure washing in an area close to other cattle and to farm workers not wearing proper protective equipment. A strict cleaning, disinfection and drying protocol is necessary to decrease the environmental contamination of pens, rooms or trailers.
For all deaths, postmortems should be performed by the herd veterinarian followed by the submission of diagnostic samples to a lab where indicated. This allows confirmation of the bacteria as well as guidance for antimicrobial treatment decisions for sick animals.
Keeping this disease under control requires reducing the environmental pressure and increasing the ability of an animal to withstand that pressure. There is currently no vaccine for Salmonella Dublin in Canada. Proper nutrition to support a healthy immune system and minimizing stressors can increase calves’ resistance to disease. Working with your herd veterinarian and nutritionist can help manage disease when it occurs.
If your herd has not had Salmonella Dublin introduced, now is the time to implement strategies to make sure it stays that way. Having a discussion with your veterinarian about cleaning products and protocols, calf treatment protocols, and biosecurity, with your nutritionist about feeding programs, and drovers and employees about hygiene standards, can help ensure your farm stays free of disease.
Follow to stay up-to-date on all Healthy Calf Conference updates. Speaker announcements, sponsorship information, registration announcements, and more.
The Codes of Practice are nationally developed guidelines for the care and handling of farm animals. They serve as our national understanding of animal care requirements and recommended practices.